“My leg started swelling and turned purple. I couldn’t walk on it and it hurt to do regular activities without the pain,” says Christie Sielfleisch, a senior and former varsity soccer goalkeeper at Rockwood Summit High School in Missouri. “I couldn’t do any contact sports. I couldn’t run, and had a really tough time putting on my jeans.”
Sielfleisch was suffering from Deep Vein Thrombosis or DVT. She had many procedures to help with the DVT. “Well, I had eight metal stents put in [vein], in order to help open it up.”
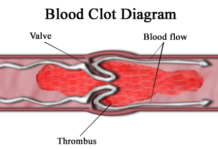
In simple terms, DVT is a blood clot in deep veins. Blood clots can form in deep or superficial veins, according to the National Institutes of Health (NIH). When the clot is in the deep vein, far from the surface of the skin, it is DVT. And when it is superficial or close to the surface of the skin, it’s called superficial thrombosis.
There are three types of DVT: acute DVT, sub-acute DVT, and chronic DVT, according to NIH. The difference between these three types is that they are ordered in chronological time; acute is new clots, sub-acute is relatively new, and chronic is old clots.
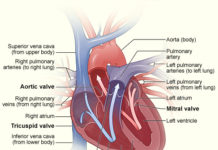
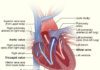
The NIH states that the most dangerous consequence of DVT is embolization or the separation of the clot, which can travel to the lungs and cause a blockage in them. This is known as a pulmonary embolism and may result in sudden death of the person.
According to the Department of Vascular and Endovascular Surgery at Loyola University Medical Center in Chicago, there are more than 200,000 cases of DVT in the United States every year. Furthermore, there are at least 50,000 cases that are complicated with pulmonary embolism.
Athletes are at a greater risk for developing DVT because of factors such as traveling long distances from sporting events, and the long term use of a brace or cast, according to stoptheclot.org—a useful website that tells you everything you need to know about DVT.
Stoptheclot.org states that “Athletes can experience a combination of both acute and superficial DVT symptoms, such as persistent calf pain or tenderness, calf or leg swelling, thigh swelling, local tenderness/pain, and erythemia (redness) at the site.”
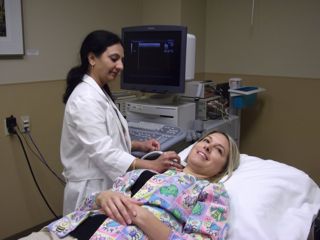
“Even though athletes are more prone to DVT, I rarely see anyone under the age of 30,” says Vijaya Vangala, a vascular sonographer at St. Lukes Hospital in Chesterfield, MO. “The people I do see are much older adults, and they are usually in the hospital for other reasons, such as surgery or other medical problems.”
Other people who are also at great risk for developing DVT include pregnant women, women who use birth control pills, people with a history of DVT in their family, cancer patients, trauma patients, and obese people, according to stoptheclot.org.
Stoptheclot.org says that DVT can be diagnosed by a doctor after discussing family medical history, physical exam of legs, and by other diagnostic tests, such as ultrasound, in which sound waves create pictures of the blood flow. Another method is venography, in which a dye is injected into the vein and an X-ray is taken. DVT can be treated with medicines such as anticoagulants, or blood thinners, and thrombin inhibitors. The inhibitors are used when patients are unable use anticoagulants, because they have bleeding problems or other medical conditions. Sielfleisch says that she mostly uses blood thinners.
In order to prevent developing a DVT, people with risk of DVT should have regular checkups, get up and walk when traveling for long hours, drink plenty of fluids, and take all medicines prescribed by your doctor. ”
“I used to get my blood drawn every week, but now it’s every 6 months,” says Sielfleisch. “I still have to go to the doctor each month for checkups to be sure that my blood levels are in check.”

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 Unported License


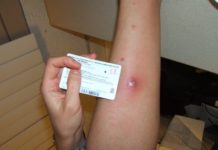
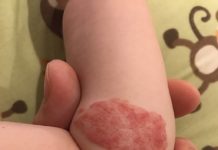






I think that this injury could have be prevented by a proper size shin gaurd. your shin gaurd must protect the enitire shin other wise it is out and exposed and easier to get kicked.